Tag: urethroplasty
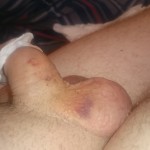
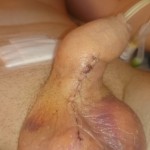
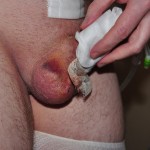
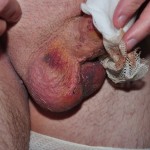
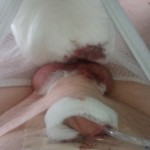
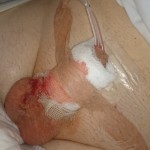
Operation day + 3 photos
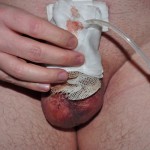
Operation day + 1 photos
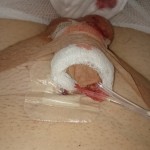
Operation day photos
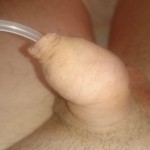
Before photos
Urethrography and discussing urethroplasty
Before I could see the senior urologist he wanted to know what he was dealing with, so I got an appointment for a cystourethrogram (x-ray of the urethra and bladder).
They’d be taking two related x-rays, a retrograde cystourethrogram (RCUG) as they squirted contrast through my urethra into my bladder and then a voiding cystourethrogram (VCUG) as I emptied my bladder.
The radiology staff didn’t seem especially familiar with the procedure, so even with a large crowd coming and going and giving advice it took over an hour. They seemed to have used too much numbing gel; every time they tried to inject the contrast the catheter would pop out.
The RCUG was eventually successful but the VCUG didn’t work so well. I found it very difficult to urinate on demand while lying on my side and having not had anything to drink for a couple of hours.
My x-ray appointment was at the end of January but I couldn’t get an appointment with the urologist until mid-March, partly because I was away quite a lot during those months.
When I finally saw the urologist he was the first doctor I’d met in the urology department with any bedside manner and he was very open to discussing the options.
I’d used the time before the appointment to continue my research and I’d found that in the few studies that actually tried to evaluate patient satisfaction buccal mucosal graft (using skin from the inside of the mouth) did better than penile flap (using skin from the penis) urethroplasty. It seems that the cosmetic results are better, there are fewer problems with skin tightness and less post-urination dribbling with the buccal mucosal graft.
The doctor would have preferred to use a penile flap and was more familiar with the technique. I had an especially awkward moment lying exposed on the examining table when he told me that there seemed to be plenty of spare skin and I had to try to explain that that’s not the case when my penis is erect.
He’d already discussed my case with a colleague in another county who had more experience with buccal mucosal grafts and we agreed that we’d go for that option and that he’d bring in his colleague to assist with the surgery.
Introduction
Like a lot of guys, I’d noticed the force of the flow when I was peeing decreasing over the years. I’d assumed it was just a normal part of getting older. In May 2014 it finally got to the point where I thought there must be something wrong. Peeing was becoming painful and the final straw was when I noticed a bit of blood.
It turned out to be a urethral stricture, scar tissue narrowing my urethra, and that diagnosis has so far resulted in lots of visits to the hospital and several surgeries: a urethrotomy (plus two failed attempts) and two buccal mucosal graft urethroplasties. In particular it was a stricture of the pendulous urethra, or distal urethra, within the external part of the penis. That seems to be quite unusual, especially when it’s not caused by disease or injury.
I’ve noticed that there’s not a lot of information out there about strictures and the treatments for them, especially from a patient’s point of view. So I’m writing this blog in the hope that it might be helpful for other guys with the same problem. If you want to get in touch with me you can use this contact form.
There are pictures to accompany some of the posts, but you’ll have to click a link to see them so that nobody unwillingly sees pictures of a penis. You can also find them in the NSFW category.